Additional resources are available from the CDC and the VDH about how to remove attached ticks. The New York Department of Health created this video about proper tick removal.
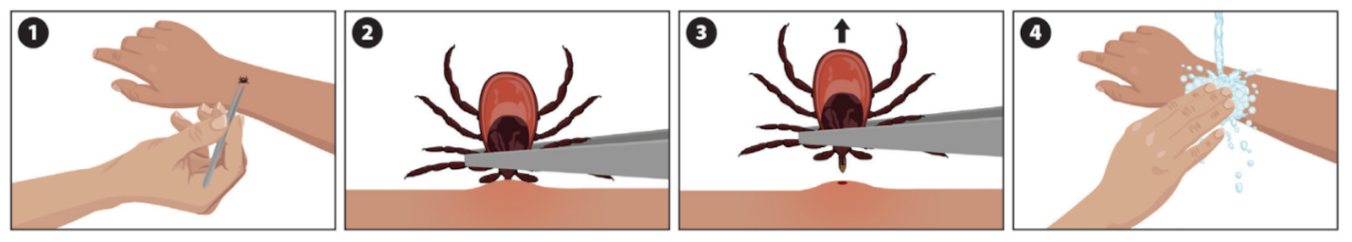
1. REMOVE THE TICK
If it’s still on you, carefully remove it. Avoid squeezing the tick’s body which can push disease causing bacteria into your body. Instead, pull from as close to your skin as possible.
- Using fine-tipped tweezers, or a tick removal tool, firmly grasp the tick as close to the skin as possible.
- With a steady motion, pull straight up until all parts of the tick are removed. Do not twist or jerk the tick. Do not be alarmed if the tick’s mouthparts remain in the skin.
- Dispose of a live tick by putting it in alcohol, placing it in a sealed bag/container, wrapping it tightly in tape or flushing it down the toilet. Never crush a tick with your fingers.
- Wash and disinfect your hands and the bite area.
Do NOT use petroleum jelly, matches, nail polish, glue, or other products to smother the tick! These methods are less effective, and may make it more likely the tick regurgitates harmful bacteria into your body.
2. IDENTIFY THE TICK
The tick to be most concerned about is the blacklegged tick (also known as the deer tick). Approximately 60% of blacklegged ticks in Vermont are infected with a disease-causing pathogen. Other ticks may also transmit disease including the Lone Star Tick, American Dog Tick, and Brown Dog Tick.
3. YOU MAY SAVE THE TICK FOR FURTHER TESTING
There are differing opinions about whether to have a tick tested for pathogens after it is removed from your body. The VDH and CDC discourage using results from these tests to guide decisions about treatment because even if a tick contains a germ, it does not mean that you have been infected. Also, a negative results can be misleading because you might have been bitten unknowingly by a different, infected tick.
Some Vermonters choose to have the tick tested immediately, or to save the tick in a plastic bag in a freezer (labeled with the date and location the tick was found and removed). If symptoms of a tickborne disease arise, testing the tick is possible when more information is needed.
4. NOTE THE AMOUNT OF TIME YOU THINK THE TICK WAS ATTACHED
The longer the tick was embedded the higher probability it will transmit an infection. However, a tick does not have to be embedded for 24 – 36 hours to transmit disease. Some TBDs can be transmitted in less than 24 hours, or (rarely but possible) in as little as 15 minutes.
5. WATCH FOR SYMPTOMS OF A TICKBORNE ILLNESS
During the early stages of Lyme disease a blood test will often remain negative while a person develops enough antibodies to be detected by the test. This means watching for signs and symptoms of illness is extremely important, because that is how Lyme and other tickborne diseases may be diagnosed in early stages when treatment is most effective.
The CDC says “During the first few weeks of infection, such as when a patient has an erythema migrans rash, the test is expected to be negative.” The CDC also notes that “Some people who receive antibiotics early in disease (within the first few weeks after tick bite) ….may only develop an antibody response at levels too low to be detected by the test.” meaning prophylactic treatment or early treatment for symptoms may result in a negative blood test, even if you are infected.
Symptoms from a tickborne infection often occur three days to 30 days after a tick bite. Symptoms of disseminated Lyme disease can occur days, months, or years after infection.
Symptoms of a TBD may include a fever, headache, “bulls-eye rash”, or joint pain. Other symptoms can include cognitive changes, gastrointestinal problems, vision changes, or insomnia. Sometimes a tickborne illness presents as a mental health disorder such as anxiety, OCD, or Depression.
6. TALK TO YOUR HEALTH CARE PROVIDER ABOUT TREATMENT OPTIONS
Because early treatment (often this may be before a blood test is positive) results in better outcomes for most TBD patients, it is important to speak to your health care provider about your treatment options as soon as symptoms start.
Some providers may recommend a full course of antibiotics when a patient from an endemic area removes an engorged tick. Other physicians may prescribe prophylactic antibiotics, although some are concerned about the limited research behind this recommendation. Some Vermonters wait to see if symptoms occur (it is important to remember that symptom onset of some TBDs may be delayed weeks, months, or years after a tick bite).
7. REMEMBER, YOU MAY NEVER SEE A TICK AND STILL CONTRACT A TICKBORNE DISEASE
Vermont is considered an endemic state for Lyme disease. According to the CDC “because tick bites are not painful, many people will not remember a tick bite” so Vermonters and their health care providers should be aware of the variety of signs and symptoms related to tickborne diseases.
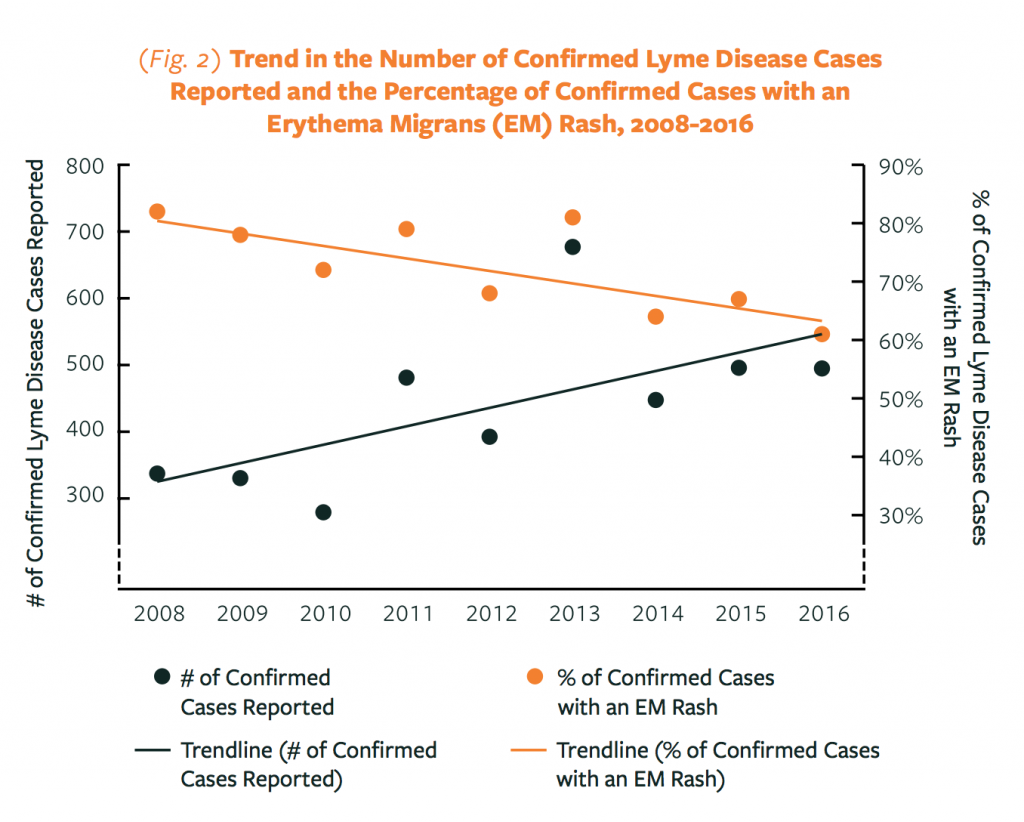
NOTE: With Lyme Disease, the Incidence of a “Bulls-Eye” Rash is Decreasing in Vermont
Many Vermonters are familiar with the “Bulls-Eye” or “erythema migrans” rash as a symptom of Lyme disease. Health care providers in Vermont should be aware that the Vermont Department of Health surveillance shows that the incidence of these rashes is decreasing in confirmed cases of Lyme disease.
Tick Identification Resources
Tick Encounter at the University of Rhode Island offers free tick identification
Vermont’s Agency of Agriculture offers free tick testing
The VT Agency of Agriculture’s Passive Tick Surveillance Program offers free identification of ticks, and monitors the distribution of ticks in the state of Vermont and tick identification images (This program does not test for pathogens)
This guide from the CDC also has images for tick identification
Tick Testing Resources
Ticknology offers a universal tick test for $25-$45. See their tick submission guidelines for how to send a tick to Ticknology
EcoLab in Massachussets tests ticks for single or multiple pathogens from $30 – $85
East Stroudsburg University’s Tick Research Lab offers tick testing for multiple pathogens. Cost is $50-$175 and are listed on the submission form
Tickreport is located at UMASS Amherst and offers several pricing packages for tick testing from $50-$200
TickCheck offers testing from $49-$200. Specific test information is on their online order form
Connecticut Veterinary Medical Diagnostic Laboratory offers tick identification and testing from $85 – $125
The Lyme Disease Lab at Stony Brook University performs tick identification with a prescription from a physician (a fee will be charged)
IGeneX tick testing costs are per pathogen as indicated on their tick test form
Thangmani Lab offers free tick testing for ticks found in NY state.